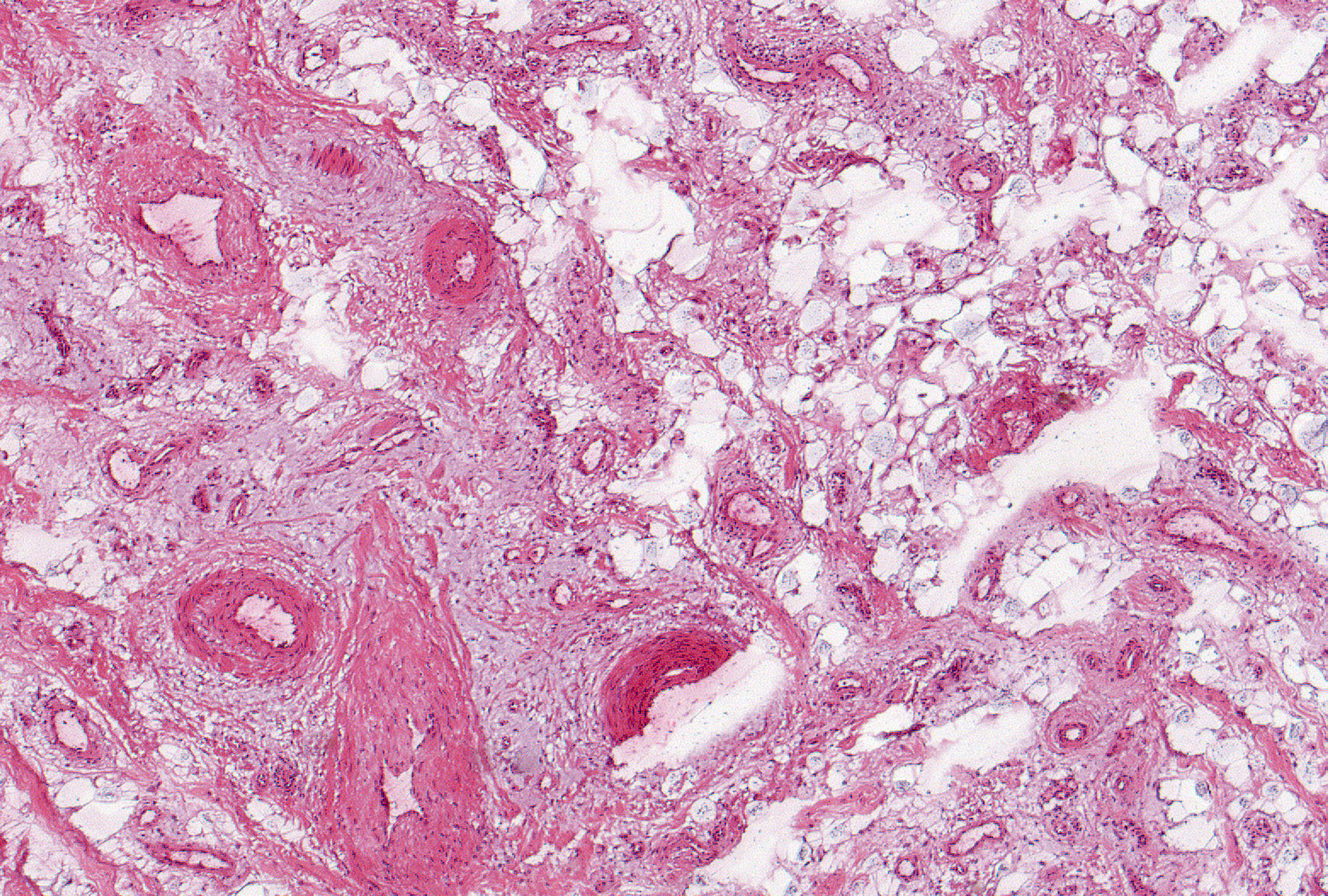
Mucous plugging, inflammation, fibrosis and obliteration of small bronchioles were histopathological features in these patients. This can be explained by resistance changes having an inverse relationship with the fourth power of the decrease in airway radius. The total airway resistance was increased in lungs from emphysema patients compared to controls, mainly due to increased small airways resistance, increasing by up to 40 fold. The small airways (< 2 mm diameter) accounted for approximately 25% of the total airway resistance in healthy controls. These observations were expanded in the landmark study by Hogg, Macklem and Thurlbeck in 1968 using a retrograde catheter technique in excised lungs from five controls and seven emphysema patients. The small airways were identified as a location causing airflow obstruction in emphysema patients. measured bronchial pressures during respiratory maneuvers in patients with emphysema and healthy controls. Overall, these changes can reduce airflow, increase gas trapping and thus reduce ventilatory capacity. This can reduce airway patency and render the airways more liable to collapse upon expiration. A loss of alveolar attachments, which radially connect to small airways like the spokes of a wheel, were also decreased in emphysematous tissue. reported mucous plugging in small airways supplying emphysematous lesions. Leopold and Gough reported narrowing of 60% of bronchioles supplying centrilobular emphysematous lesions. A striking feature of these studies is the heterogeneity of changes reported, including inflammation, fibrosis, narrowing, dilatation and obliteration of bronchioles. Histopathological evidence of SAD in COPD gained momentum in the mid-twentieth century Table 1 lists the major findings of studies spanning from 1953 to 1971. “ I am prepared, then, to maintain, that emphysema of the lung may, in all cases which I have witnessed, be satisfactorily accounted for by considering it as a secondary mechanical lesion, dependent on some condition of the respiratory apparatus leading to partially diminished bulk of the pulmonary tissue, and consequently disturbing the balance of air in inspiration.” We discuss the mechanisms which cause SAD progression, including bacterial colonization and exacerbations. We focus on clinically relevant topics, including the relationship between SAD and emphysema, and SAD in the early stages of COPD. We give a historical overview of key studies regarding the nature of SAD in COPD, and describe the various pathological features of SAD. This article provides a comprehensive review of the pathology of SAD in COPD. Small airway disease (SAD) is a key feature of COPD, and has been studied extensively over many decades. It is estimated that 20% of small airways below 2 mm diameter comprise bronchi with elements of cartilage within their walls, while the remainder are bronchioles or alveolar ductal spaces. The small airways have been defined as < 2 mm diameter and arise from the 4th – 13th generation of airway branching (taking trachea as 1st generation to alveoli as 23rd), but on average arise by the 8th. The narrow diameter of the peripheral airways means that particles can more easily collide with the surface and cause damage compared to the larger airways. The burning of tobacco cigarettes produces a complex mixture of chemicals and gases capable of reaching the alveoli. Chronic obstructive pulmonary disease (COPD) is caused by the harmful effects of cigarette smoking, or other noxious particles, resulting in persistent airflow limitation and symptoms including dyspnoea, cough and sputum production.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
